Posterior Tibial Tendon Dysfunction, Posterior Tibial Tendinitis
Watch the video above to learn about Posterior Tibial Tendon Dysfunction, Posterior Tibial Tendinitis, and how I approach treating this with my patients. There's also more information below. As always, when you're ready, fill out the form on this page to request a consultation.
He spent a lot of time with me, and the time that he spent was invaluable as he explained everything in great detail in terms that I was able to understand. – Kelvin
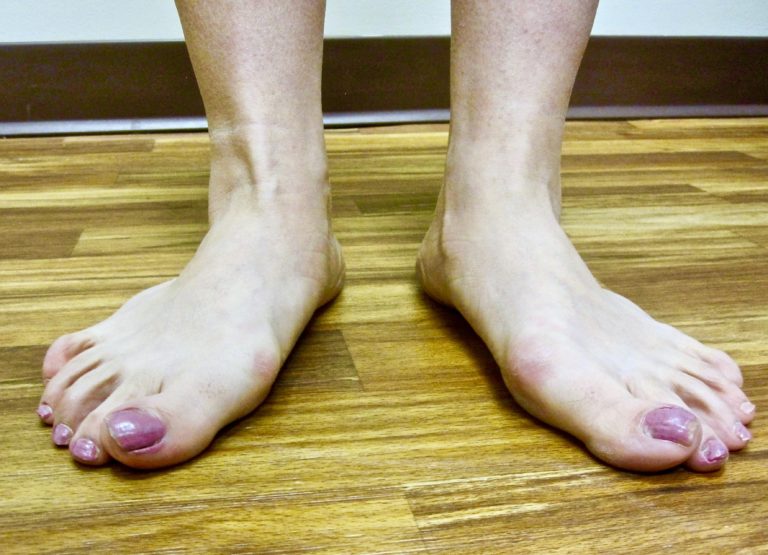
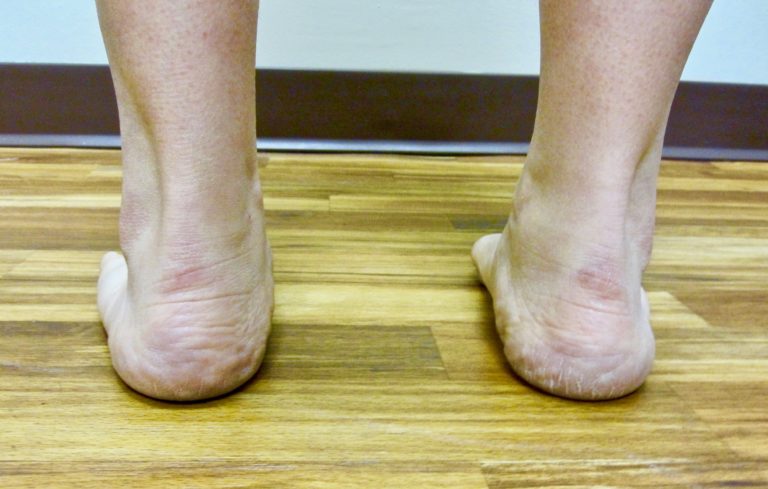
Posterior tibial tendon dysfunction also known as posterior tibial tendinitis is a condition that occurs when there is inflammation along the tendon sheath and/or tears along a portion of the tendon. This can result in the inability of the tendon to support the arch of the foot. Advanced posterior tibial tendon dysfunction can result in a rigid adult acquired flatfoot deformity.
Symptoms
- Pain is commonly felt approximately 2 cm above the ankle bone (medial malleolus), yet it can also occur anywhere along the course of the tendon including at the insertion of the tendon into the navicular bone on the inside of the foot
- Swelling
- Tenderness along the tendon
- Progressive flattening of the foot
- Pain on the top and outside of the foot and/or ankle along the subtalar joint or lateral ankle respectively
- Spasm of the peroneal tendons on the outside of the foot and ankle
- Heel pain
- Pain along the tarsal tunnel (similar to the carpal tunnel in the hand)
Diagnosis
Diagnosis is made by a comprehensive foot and ankle exam by Dr. Stewart along with x-rays of the foot. Imagining studies such as ultrasound and MRI are sometimes required to determine the extent of tendon injury.
Treatment
Posterior tibial tendon dysfunction generally takes 6-8 weeks to improve and early activity on a healing tendon can result in a set back in recovery. Non-compliance can double the recovery time and can be very frustrating for patients.
Posterior tibial tendon dysfunction is a progressive condition. Early and aggressive conservative treatment can prevent posterior tibial tendon dysfunction from advancing to an adult acquired flat foot deformity. Dr. Stewart terms posterior tibial tendon dysfunction a pro-active condition. Although we can never offer a 100% guarantee, the majority of Dr. Stewart’s patients improve with conservative (non-surgical care).
With the confidence Dr. Stewart had in his work I knew this was the best option for me. It was a “no brainer.” We had to do it. Dr. Stewart answered every question that me and my family had. He took the time to explain the operation, the recovery, and the physical rehabilitation that I would be going through. Dr. Stewart guided me through the whole process. -Chris Schrader
Conservative treatment for Posterior Tibial Tendon Dysfunction – Posterior Tibial Tendinitis includes:
- Immobilization of the foot and/or ankle. Depending on the severity of the condition, this may require cast immobilization with crutches, a walking boot, a hinged ankle foot orthosis with supportive shoe gear, a multi-ligamentous ankle brace with supportive shoe gear, or custom foot orthotics with supportive shoe gear
- Modification of physical activity including avoidance of walking, jogging, running, and the elliptical for exercise. Recommended exercises include circuit training, swimming, and bicycling
- Stretching and strengthening exercises with a Theraband and/or with single and double limb heel rise
- Therapeutic laser
- Compression therapy generally with prescription compression stockings
- Physical therapy
- Weight loss and dieting
- Medications including anti-inflammatory medications (NSAIDs), Tylenol, oral steroids, and in some cases narcotic pain medication
- Ice along the tendon 2-3 times per day for 20 minutes at the area of maximum tenderness. Elevation is recommended while icing
- Avoidance of flip-flops, flats, and barefoot walking
- Supportive shoe gear including a motion control running shoe such as Brooks, Asics, New Balance, or Saucony. Keen and Merrell style shoes are also recommended
- Custom foot orthotics
- Steroid injections into foot and/and or ankle joints
If all conservative intervention fails, then surgical intervention maybe required. Dr. Stewart will determine which procedure is best for you.
Surgical treatment for Posterior Tibial Tendon Dysfunction – Posterior Tibial Tendinitis includes:
- Debridement and repair of the tendon with tendon advancement
- Tendon transfer
- Reduction of a hypertrophic navicular bone or removal of an accessory navicular bone
- Cutting of bone (osteotomy) and fixation with screws
- Subtalar joint implant
- Joint fusions (arthrodesis)
